Understanding Heart Rate Variability: When Change Actually Means Something
The internet has become full of discussions about Heart Rate Variability. It’s sometimes treated as the holy grail of longevity and wellness, but what is it and why should we care about measuring it?
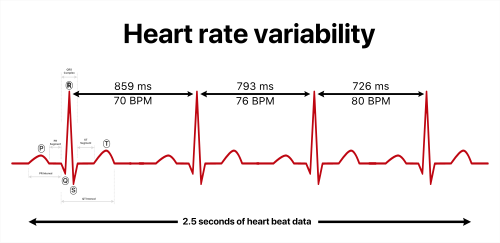
Heart Rate Variability—or HRV—is essentially the variation in time between consecutive heartbeats. Somewhat like the difference between runners on a trail - they may look evenly spaced, but there is often a little bit more or less distance between them. Counterintuitively, a more variable heart rate (within reason) is generally better. It reflects your autonomic nervous system’s ability to respond to stress and recovery flexibly. When your parasympathetic (”rest and digest”) system is dominant, HRV tends to be higher. When you’re stressed, sick, overtrained, or sleep-deprived, it typically drops.
The appeal is obvious: a single morning measurement that supposedly tells you whether to push hard or rest. But here’s the problem—HRV is maddeningly noisy, and most people misinterpret what they’re seeing.
HRV Isn’t Just Wellness Theater
HRV has been studied in a variety of settings, and it’s not just biohacker hype. In healthcare, it’s perhaps best known through the work of Randall Moorman and the development of the HeRO (Heart Rate Observation) score, which showed that declining HRV in premature neonates was an early warning sign of sepsis—often appearing hours before conventional vital signs changed.[1] This kind of physiologic monitoring has real clinical utility in acute care settings.
So while tracking your morning HRV to decide whether to do interval training might seem like a fool’s errand compared to predicting neonatal sepsis, we know the underlying physiology is real. The question is: can we actually use it meaningfully in health and wellness contexts, where the signals are subtler and the noise is everywhere?
I think the answer is yes—but only if we’re patient and honest about the limitations.
A Quick Note on Metrics
When we talk about HRV, we’re usually referring to rMSSD (root mean square of successive differences). It’s a mouthful, but it’s simply a mathematical way of quantifying the beat-to-beat variation in your heart rate, measured in milliseconds. Most consumer devices—your Oura Ring, Whoop, Apple Watch—use rMSSD or similar time-domain metrics because they’re reliable even with short measurement windows.
You might also see SDNN (standard deviation of all intervals) or frequency-domain measures, but rMSSD has become the standard for daily tracking because it specifically captures parasympathetic activity and doesn’t require five-minute measurements.[2]
Higher numbers generally mean better autonomic flexibility, but—and this is critical—your baseline is uniquely yours. An athlete might have an rMSSD of 100+ ms while someone else is perfectly healthy at 30 ms. It’s the trend and response pattern that matters, not the absolute number.
Why HRV Is So Variable
HRV fluctuates day to day due to:
Sleep duration and timing
Acute stress (psychological and physiologic)
Alcohol consumption
Illness or subclinical inflammation
Training load (especially eccentric or high-intensity work)
Measurement conditions (time of day, posture, device algorithm)
Single-day or even 2–3-day changes are almost never meaningful on their own. Yet I see people constantly adjusting their lives based on one bad reading. That’s like checking your weight once and declaring your diet has failed.
The Time Horizons That Actually Matter
1. Establish a Baseline (2–4 weeks minimum)
Before you can know if something is working, you need to know what’s normal for you. This means measuring consistently—same time of day, same posture (I recommend supine, right after waking), same device and metric (rMSSD is most common).
Three to four weeks captures your natural rhythm: weekday versus weekend patterns, normal stress oscillations, your typical training load. Without this, you’re flying blind.[3]
2. Short-Term Effects (1–7 days)
This is the acute response window. Your HRV might drop after starting a new training program or spike after a meditation session. These are responses, not adaptations.
A temporary drop after hard training? Expected. A sustained drop over weeks despite adequate recovery? That’s a different signal. Don’t confuse the two.
3. Medium-Term Adaptation (3–6 weeks)
This is where most interventions can actually be evaluated. Whether you’re improving your sleep, reducing alcohol, starting endurance training, or beginning CPAP therapy, you need at least this much time to see if the autonomic nervous system is truly adapting.
What you’re looking for isn’t just higher numbers—it’s a shift in your rolling baseline, reduced day-to-day volatility, and better recovery after stressors. The system is becoming more resilient, not just occasionally higher.[4]
4. Long-Term Remodeling (8–12+ weeks)
This is where real autonomic set-point changes happen. Your HRV doesn’t just spike higher on good days—the floor rises. You rebound faster after stress. Previously challenging stressors no longer suppress your HRV as much.
This matters for endurance athletes, people recovering from chronic illness, aging interventions, or anyone trying to fundamentally shift their autonomic balance. It requires patience.[5]
How to Actually Analyze HRV
Forget single-day values. Use rolling averages—a 7-day average for short-term trends, 14–28 days for true baseline shifts.
A real improvement looks like:
Rising mean HRV over weeks
Decreasing day-to-day variability
Faster rebound after poor sleep or hard efforts
Resilience to stressors that used to tank your numbers
A false signal looks like:
Sporadic spikes with no pattern
Improvement only on rest days
Gains that disappear with minimal stress
A useful statistical heuristic: a change of roughly 0.3–0.5 standard deviations from baseline, sustained over 2–3 weeks, is likely meaningful for you as an individual.[6]
My Practical Recommendation
If you’re running this as an experiment on yourself:
Baseline: 3–4 weeks of consistent measurement
Intervention: Minimum 4–6 weeks
Analysis: Compare the last 2 weeks of baseline against the last 2 weeks of intervention using rolling averages
If the signal persists despite normal life chaos—work stress, travel, occasional poor sleep—it’s probably real.
Bottom Line
Days: noise
1–2 weeks: acute response
3–6 weeks: adaptation signal
8–12+ weeks: true autonomic remodeling
HRV rewards patience and humility—and punishes over-interpretation. The data is useful, but only if you resist the urge to react to every fluctuation. Measure consistently, think in weeks not days, and remember that the goal isn’t perfect numbers—it’s a system that adapts and recovers well over time.
That kind of resilience doesn’t show up overnight.
References
[1] Moorman JR, Carlo WA, Kattwinkel J, et al. Mortality reduction by heart rate characteristic monitoring in very low birth weight neonates: a randomized trial. J Pediatr. 2011;159(6):900-906.e1.
[2] Shaffer F, Ginsberg JP. An overview of heart rate variability metrics and norms. Front Public Health. 2017;5:258.
[3] Plews DJ, et al. Training adaptation and heart rate variability in elite endurance athletes: opening the door to effective monitoring. Sports Med. 2013;43(9):773-781.
[4] Attia P. Heart rate variability: what is it and how do we use it? Peter Attia Drive Podcast. https://peterattiamd.com/ama-hrv/
[5] Huberman A. Using your nervous system to enhance your immune system. Huberman Lab Podcast. https://www.hubermanlab.com/episode/using-your-nervous-system-to-enhance-your-immune-system
[6] Nakamura FY, et al. Intraday and interday reliability of ultra-short-term heart rate variability in rugby union players. J Strength Cond Res. 2017;31(2):548-551.